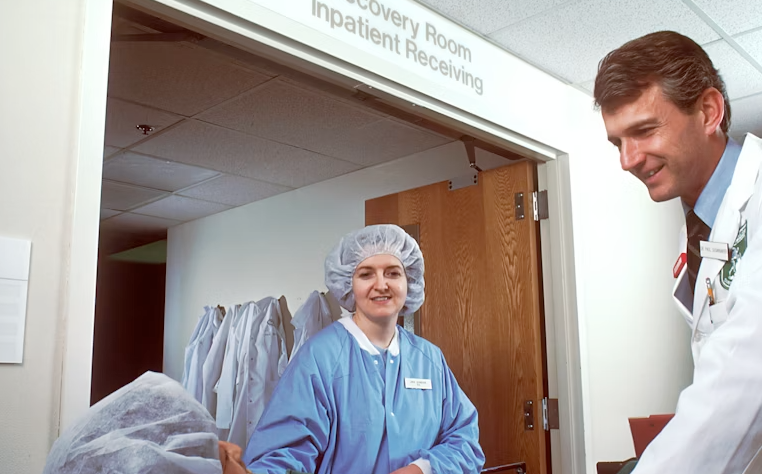
Many patients leave appointments with prescriptions in hand but still feel unsure about what to do next. Some hesitate to ask questions. Others forget instructions the moment they step outside the clinic. This gap between treatment and understanding often slows recovery more than the illness itself. Healing depends on more than medication or procedures. It depends on how patients feel during the process—whether they feel heard, supported, and guided.
Small actions from healthcare providers and caregivers can change that experience completely. They help patients stay calm, follow instructions correctly, and trust the process. In this article, we’ll look at practical, real-world ways simple acts of care can improve recovery in meaningful ways.
Listening Like It Actually Matters
Patients can tell when someone is only half paying attention. A rushed tone or constant typing during a conversation makes them hold back important details. Good listening changes that dynamic. When a provider pauses, makes eye contact, and lets the patient finish speaking, the quality of information improves right away. Patients mention symptoms they almost skipped. They explain concerns more clearly. This helps avoid misunderstandings that can delay proper treatment. Listening also builds trust. A patient who feels heard is more likely to follow advice and return for follow-ups.
Helping Patients Stay Organized Day to Day

Recovery often comes with multiple instructions, medications, and follow-up appointments. Patients can easily feel overwhelmed, especially if they are managing everything alone. Clear organization helps them stay on track. Writing down instructions, giving simple schedules, and explaining what needs priority can prevent confusion at home. Many patients forget verbal instructions, so having something they can refer to makes a real difference. This is where trained staff, including those with medical assistant college degrees, play an important role in guiding patients through daily care routines. When patients understand how to manage their day, they make fewer mistakes with medication and appointments. Consistency improves, and recovery becomes more predictable instead of stressful and uncertain.
Remembering the Little Things About Patients
Patients notice when they are treated like individuals instead of case files. Remembering small details—like a past concern, a recent test, or even how someone felt during their last visit—creates a sense of continuity. It shows that their experience matters beyond a single appointment. This approach helps patients feel more comfortable sharing updates, including things they may have been hesitant to mention before. It also reduces repetition, which can be frustrating during frequent visits. When patients feel recognized, they engage more openly. That openness leads to better communication and more accurate care. Over time, this kind of attention builds a stronger relationship, which supports long-term recovery and better overall health management.
Explaining Care in Plain, Everyday Language
Medical terms can confuse patients, even when they nod along during appointments. Many leave without fully understanding what they were told. Clear communication solves this problem quickly. When instructions are explained in simple, direct language, patients know exactly what to do at home. They understand how to take medication, when to rest, and what signs to watch for. This reduces mistakes that can slow recovery or lead to complications. It also gives patients confidence. They feel more in control of their situation instead of guessing their way through it. Good communication includes checking if the patient understands, not just asking if they do. That small step makes a noticeable difference in how well instructions are followed.
Creating a Space That Feels Safe and Calm
The environment around a patient affects how they respond to care. A noisy, disorganized space can make someone feel uneasy before treatment even begins. On the other hand, a calm and respectful setting helps patients relax and stay cooperative. Simple things like a clean room, a quiet tone, and clear explanations of what will happen next can ease tension quickly. Privacy also plays a role. Patients open up more when they feel their concerns are handled with care and discretion. When stress levels drop, communication improves and procedures become easier to manage. This creates a better overall experience, which supports both emotional comfort and physical recovery.
Checking In After the Visit Ends
Care should not feel like it stops once a patient walks out the door. A quick follow-up can make a strong impact on how someone manages their recovery. Patients often think of questions later or notice symptoms they did not mention earlier. A simple call or message gives them a chance to clarify things without waiting for the next appointment. It also helps catch issues early, before they become serious. This kind of attention shows patients that their progress matters. It encourages them to stay consistent with their treatment plan. When patients know someone is checking in, they feel supported and are more likely to stay engaged in their recovery process.
Supporting the Emotional Side of Recovery
Physical symptoms often get full attention, while emotional strain stays in the background. Patients deal with fear, frustration, and uncertainty, especially during long treatments. These feelings can affect sleep, appetite, and motivation to follow care plans. A few moments of reassurance can ease that burden. Simple phrases like “this is expected” or “you’re on the right track” help patients feel steady. Asking how they are coping, not just how they feel physically, opens better conversations. When patients feel emotionally supported, they stay more consistent with treatment and communicate more honestly. This leads to better decisions and fewer setbacks. Emotional care does not require extra tools. It requires awareness and a willingness to engage beyond symptoms.
Respecting Time, Privacy, and Personal Boundaries
Patients value their time and personal space, especially when they are already dealing with discomfort. Long waits without updates can increase frustration and anxiety. Keeping patients informed about delays helps manage expectations. During appointments, asking for consent before exams or procedures shows respect and builds trust. Maintaining privacy during conversations encourages patients to speak openly about sensitive issues. Clear boundaries also help patients feel safe, especially in unfamiliar settings. These actions may seem routine, but they shape how patients experience care. When people feel respected, they engage more honestly and cooperate better with treatment. This leads to clearer communication and more effective care throughout the recovery process.
Recovery depends on consistent care, clear communication, and trust between patients and healthcare providers. Small actions shape how patients feel, how well they follow instructions, and how confident they are in their treatment. Listening carefully, explaining clearly, and staying attentive to emotional needs all contribute to better outcomes. These steps do not require extra time or advanced tools. They require awareness and intention during everyday interactions. When patients feel supported and understood, they take a more active role in their recovery. That involvement leads to fewer mistakes, better follow-through, and a smoother path back to health. In the end, steady, thoughtful care often makes the biggest difference.